DENTISTRY & CORONA VIRUS– WHAT’S THE NEW NORMAL?
Among all health care professionals, Dentists are one of the worse affected and are deeply concerned because of the COVID – 19.
In these unprecedented and extraordinary circumstances Dentistry has been badly hit and this certainly calls for defining new protocols of Safe Practice. As a health care professional, it is up to the Dentists to make well-informed decisions about their patients and practice.
Various Dentists and Dental Practices are echoing their apprehension over the future of Dentistry. Dentistry has always been under-rated and one of the cheapest in India, because of which it becomes nearly impossible to standardize the quality and standards of Dental Services.
There is also a majority of Practice who have been following high standards of quality and hygiene and are already preparing themselves to survive the pandemic and continue to help their patients with best dental services while keeping their doctors and their patients fully protected.
While all routine Dental Services and examination has been suspended until the lockdown however, it is also certain that this is not going to end anytime soon even after the lockdown, so what is going to be the NEW NORMAL for Dentists and how are Dentists going to survive?
Why are Dentists at risk and Dentistry so vulnerable?
Direct or Indirect Transmission: As per WHO and advisory by IDA the virus can be passed directly from person to person by respiratory droplets; emerging evidence suggested that it may also be transmitted through contact and fomites. Dental patients and professionals can be exposed to pathogenic microorganisms, including viruses and bacteria that infect the oral cavity and respiratory tract. Dental care settings invariably carry the risk of infection due to the specificity of its procedures, which involves face-to-face communication or direct transmission (cough, sneeze, and droplet inhalation transmission) and contact transmission (contact with oral, nasal, and eye mucous membranes). In addition, studies have shown that respiratory viruses can be transmitted from person to person through direct or indirect contact, or through coarse or small droplets, and 2019-nCoV can also be transmitted directly or indirectly through saliva.
Dental care settings invariably carry the risk of 2019-nCoV infection due to the specificity of its procedures, which involves face-to-face communication with patients, and frequent exposure to saliva, blood, and other body fluids, and the handling of sharp instruments. The pathogenic microorganisms can be transmitted in dental settings through inhalation of airborne microorganisms that can remain suspended in the air for long periods, direct contact with blood, oral fluids, or other patient materials, contact of conjunctival, nasal, or oral mucosa with droplets and aerosols containing microorganisms generated from an infected individual and propelled a short distance by coughing and talking without a mask, and indirect contact with contaminated instruments and/or environmental surfaces.
How to minimize chance of exposures?

In the light of WHO declaring the COVID-19 virus to be a pandemic, the Indian Dental Association (IDA) recommends preventative measures for dental professionals to minimize transmission through contact and dental procedures --- as scientific information leads to improvements in infection control, risk assessment, and disease management.
- Post a sign at the entrance to the dental practice which instructs patients having symptoms of a respiratory infection (e.g., cough, sore throat, fever, sneezing, or shortness of breath) to please reschedule their dental appointment and call their physician. The same thing applies if they have had any of these symptoms in the last 48 hours.
- Reschedule appointments if your patients have traveled outside India in the last two weeks to an area affected by the coronavirus disease. This includes China, Hong Kong, Iran, Italy, France, Spain, Germany, Japan, Singapore, South Korea, Taiwan, Thailand, Vietnam or any other COVID19 affected country.
- Take a detailed travel and health history when confirming and scheduling patients. Do not provide non-emergent or cosmetic treatment to the above patients and report them to the health department immediately. Screen patients for travel and signs and symptoms of infection when they update their medical histories.
- Incorporate questions about new onset of respiratory symptoms into daily assessments of all patients.
- Take temperature readings as part of the routine assessment of patients before performing dental procedures.
- Take the contact details and address of all patients treated.
- Install physical barriers (e.g., glass or plastic windows) at reception areas to limit close contact with potentially infectious patients.
- Make sure the personal protective equipment being used is appropriate for the procedures being performed.
- Use a rubber dam when appropriate to decrease possible exposure to infectious agents.
- Use high-speed evacuation for dental procedures producing an aerosol.
- Autoclave handpieces after each patient.
- Have patients rinse with a 1% hydrogen peroxide solution before each appointment.
- Clean and disinfect public areas frequently, including door handles, chairs and bathrooms.
- Post visual alerts icon (e.g., signs, posters) at the entrance and in strategic places (e.g., waiting areas, elevators, cafeterias) to provide patients with instructions (in appropriate languages) about hand hygiene, respiratory hygiene, and cough etiquette. Instructions should include how to use tissues to cover nose and mouth when coughing or sneezing, to dispose of tissues and contaminated items in waste receptacles, and how and when to perform hand hygiene.
- Provide supplies for respiratory hygiene and cough etiquette, including alcohol-based hand rub (ABHR) with 60-95% alcohol, tissues, and no-touch receptacles for disposal, at entrances, waiting rooms, and patient check-ins.
Facial Protection
Wear a surgical or procedure mask and eye protection (face shield, goggles) to protect mucous membranes of the eyes, nose, and mouth during activities that are likely to generate splashes or sprays of blood, body fluids, secretions, and excretions.
Gown
Wear to protect skin and prevent soiling of clothing during activities that are likely to generate splashes or sprays of blood, body fluids, secretions, or excretions
Linens
Handle, transport, and process used linen in a manner which: prevents skin and mucous membrane exposures and contamination of clothing.
Avoids transfer of pathogens to other patients and or the environment.
A comprehensive details on “Guidelines for Dental Professionals on the Coronavirus Threat” can be read here.
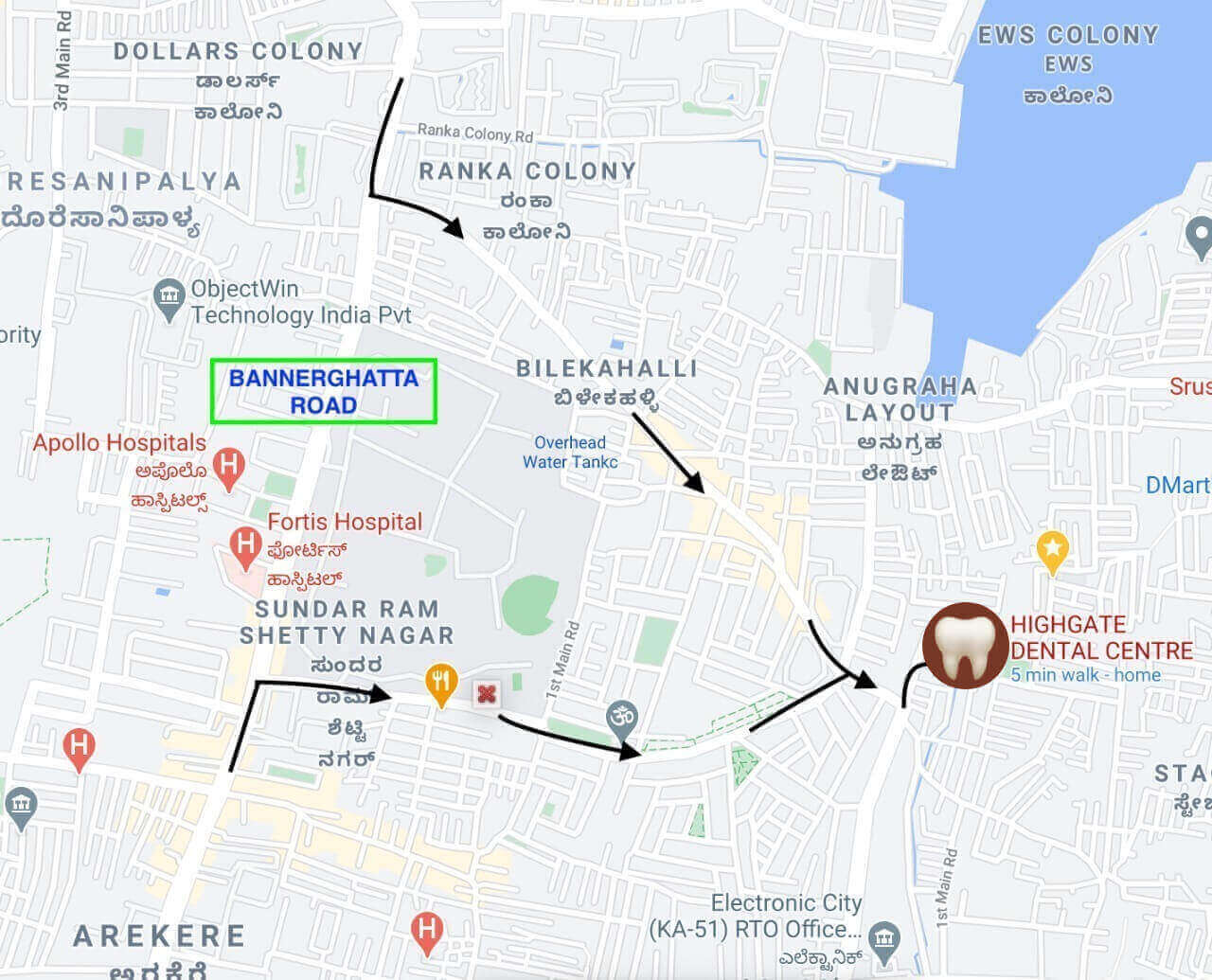
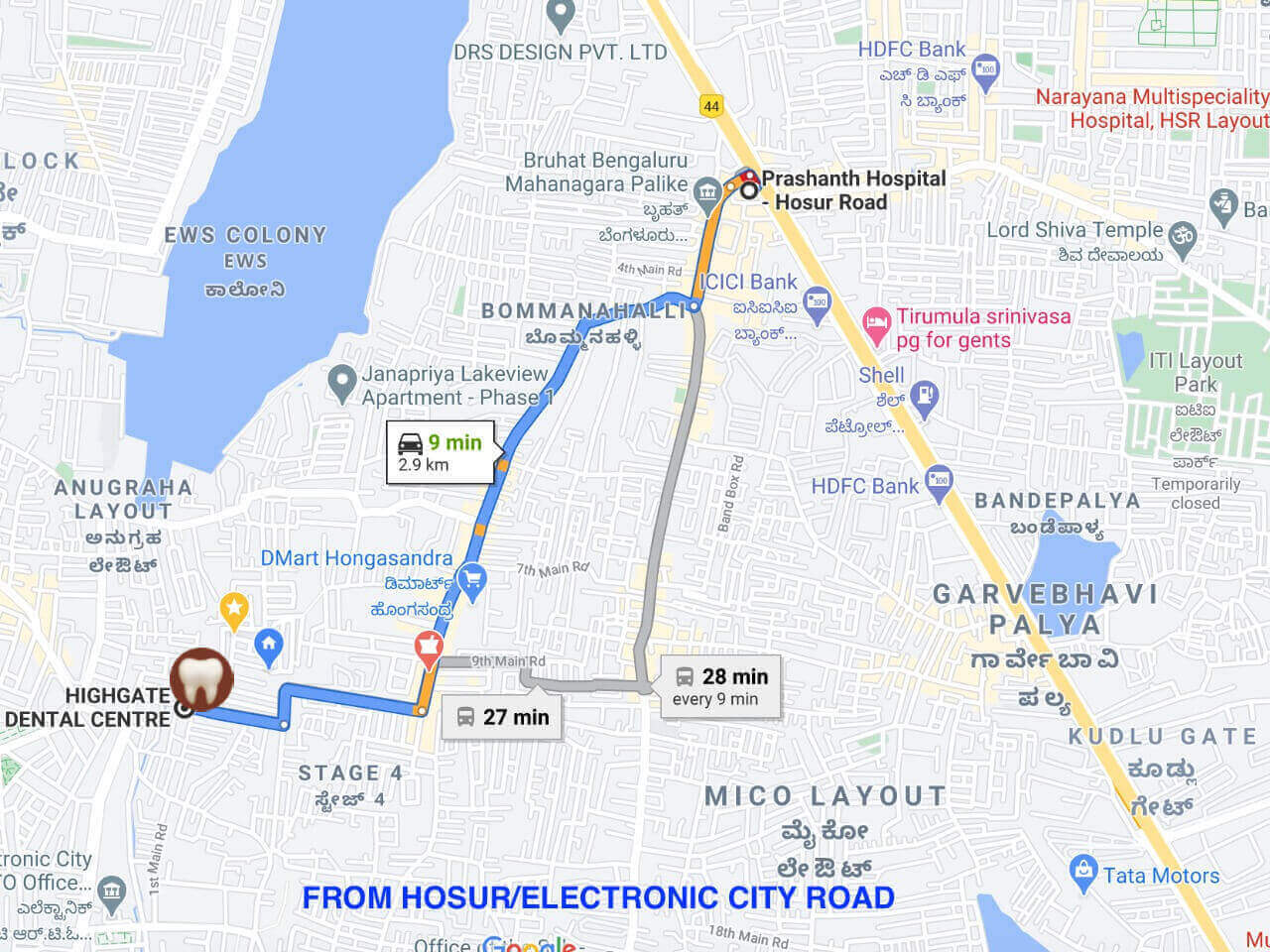
We at Highgate Dental Centre are committed to follow all the guidelines as directed and cannot compromise with the safety of our patients and our staff at any cost. We request all our readers and fellow Dentists to ensure we as a society are following it for the safe future of Dentistry and well-being of our patients.
This is the NEW NORMAL which every Patient and Dentists must be open to and accept it for a very long time in the coming years ahead.
We hope when the instant Corona Virus Test kits are available, it will become mandatory for patients to get it done before an appointment. This will certainly make the practice even more secure and doctors confident to work.